Protecting sight in an ageing, diabetic world
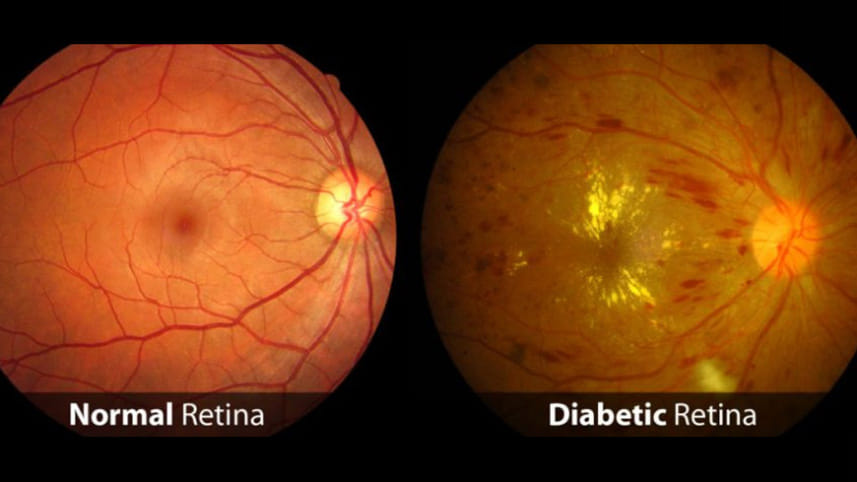
As populations age and lifestyle-related diseases such as diabetes become more prevalent, disorders of the retina are emerging as a major public health concern worldwide. During his recent visit to Dhaka, Clinical Associate Professor Doric Wong, a Singapore-based ophthalmologist and retinal specialist, spoke to The Daily Star about common retinal diseases, advances in eye care, and why early screening can save sight.

What are the most common retinal diseases you see today, and why are they increasing?
Two retinal conditions are becoming particularly common: age-related macular degeneration (AMD) and diabetic retinopathy. AMD is, unfortunately, a consequence of people living longer. As societies age, the central part of the retina—the macula—gradually becomes unhealthy. In its milder form, known as dry AMD, there is slow thinning and degeneration. In more aggressive forms, abnormal blood vessels grow, leak, and bleed, leading to sudden and severe loss of vision.
Diabetic retinopathy, on the other hand, reflects the rising prevalence of diabetes worldwide. As countries develop and lifestyles change, more people develop diabetes. If blood sugar levels are poorly controlled over time, the small blood vessels in the retina are damaged, leading to vision loss.
How far has retinal surgery advanced in recent years?
There has not been a single dramatic breakthrough, but rather steady, meaningful progress. Surgical instruments have become much finer, microscopes and visualisation systems far more advanced, and overall procedures safer and more precise. These step-by-step improvements make surgery less invasive and reduce complications.
While technologies such as robotics have been discussed for years, retinal surgery still relies heavily on the precision of the human hand. At present, nothing has surpassed that.
Can retinal diseases be detected before vision is lost?
Yes—and this is critically important. Many early retinal diseases cause no symptoms at all. Diabetic retinopathy, in particular, can progress silently until vision is already compromised.
That is why screening is so effective. In many countries, people with diabetes undergo annual retinal photography. Increasingly, artificial intelligence is being used to screen these images and identify early disease. Patients only need to see a specialist if changes are detected, making the system both efficient and cost-effective.
Once vision is lost, it is often difficult to restore fully—so early detection is key.
How effective is artificial intelligence in eye disease detection today?
AI holds enormous promise, but implementation takes time. Although AI-based systems have been discussed for years, only a limited number have been formally approved for clinical use. That said, AI is already helping to identify retinal disease in large-scale screening programmes and will play an increasingly important role in the future.
What is the success rate of retinal surgeries such as retinal detachment repair?
Retinal detachment occurs in about one in 10,000 people. If detected early and treated promptly, the first surgery is successful in about 85–90 per cent of cases. Some patients require additional procedures, but overall outcomes are very good when managed by trained specialists.
Diabetes can also cause retinal detachment, but through a different mechanism involving bleeding and scarring inside the eye.
Which is more common: cataract or retinal disease?
Cataract is by far the most common cause of vision impairment, and it is largely age-related. There is limited scope for prevention beyond general eye protection.
The good news is that cataract surgery is one of the most successful operations in modern medicine. In around 98–99 per cent of cases, vision is restored to near-normal levels. Unlike many other surgeries, cataract surgery often allows patients to return to full visual function.
What warning signs should prompt people to seek eye care?
Blurred vision that cannot be corrected with glasses is an obvious sign. However, some conditions—particularly glaucoma—are more dangerous because they progress silently.
Glaucoma is often called the “thief of sight” because it gradually damages peripheral vision without the patient noticing. Those with a family history of glaucoma should be screened regularly, especially after the age of 40.
How does eye care in Bangladesh compare with Singapore?
From what I have seen, Bangladesh has the necessary technology, medications, and skilled professionals to manage most eye conditions. Modern retinal surgery equipment and treatments for diseases such as AMD are available here.
The main challenges are access and availability, particularly in rural areas, as well as economic factors. Patients who travel abroad often do so for reassurance rather than because care is unavailable locally.
What makes Singapore a leader in retinal care?
Singapore is at the forefront of medical retina research, particularly in the treatment of age-related macular degeneration and diabetic retinopathy. Many new drugs and treatment protocols are developed and tested through research conducted there. These advances eventually benefit patients globally, including those in South Asia.
Your key message for readers?
Vision loss from many eye diseases is preventable. Regular eye examinations—especially for people with diabetes or a family history of eye disease—can protect sight. Once vision is lost, recovery becomes far more difficult. Early action truly makes a difference.



 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel.
Comments