Where do medical assistants fit into our health system?
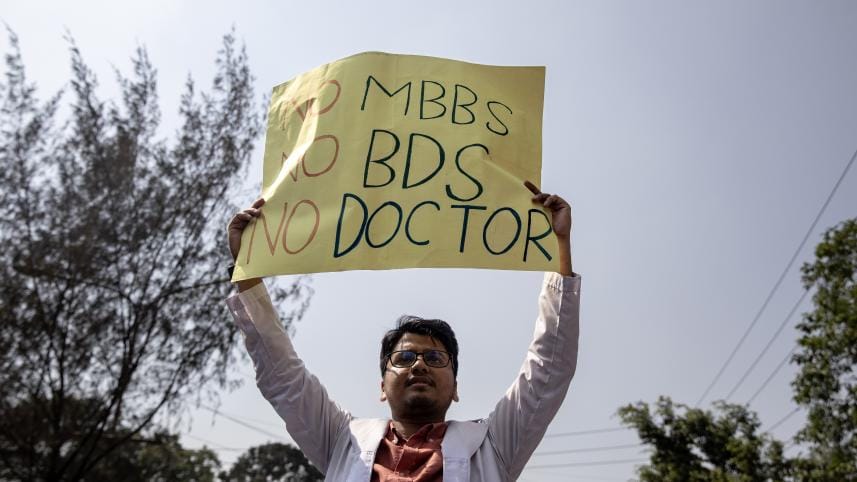
Healthcare is a collaborative exercise. Healthcare professionals of different levels and qualifications work under the same system to provide patients with optimised healthcare. However, a lack of clear demarcation within the infrastructure and the transgression of existing boundaries by medical assistants, in particular, have led to controversy and widespread protests across the country.
In what capacity have Diploma Medical Practitioners been working?
There are currently 16 government-run Medical Assistant Training Schools with over 200 non-government MATS-related institutes. These schools offer a Diploma in Medicine Faculty (DMF) course of three years with a year's internship. The qualification required to get into one of these schools is a minimum 2.5 GPA in SSC or equivalent exams.
According to the Bangladesh Medical and Dental Council (BMDC) Act of 2010, the BMDC recognises MATS as 'medical assistants'. It also has strict guidelines for the 73 drugs they can administer and the minimal external surgeries they can perform (under the supervision of a qualified doctor, of course).

Following these guidelines, they can apply to work as Sub Assistant Community Medical Officers (SACMO) under the Directorate General of Health Services (DGHS) at different NGOs, or practice privately in remote areas. Registered Medical Practitioners (RMP) or Local Medical Assistant and Family Planning (LMAFP) are entirely separate courses, requiring 3 to 8 months to complete. These degrees, producing "village doctors", are less regulated. Moreover, applicants can range from SSC graduates to postgraduates in any subject. This degree is, however, not recognised by the BMDC.
Why is it a risk to public healthcare?
In August 2024, the BMDC ruled that Diploma Medical Practitioners can use the title "Dr" before their names. The use of "Dr" has given rise to widespread condemnation from the MBBS community, claiming that the rural populace often cannot differentiate between an MBBS doctor and a DMF doctor. They see the prefix "Dr" and immediately feel a sense of security. Many DMF doctors, capitalising on this trust, do not adhere to the 73-drug list published by the BMDC and perform complex surgeries or even cesarean sections without supervision.
Moreover, medical assistants prescribing ultrasonography of the uterus in male patients and antibiotics for more than three months have sparked widespread outrage on social media. There is no international precedent for paramedics or medical assistant equivalents to use "Dr". But MATS students continue to demand that they should be allowed to practice as diploma doctors because they've gone through four years of schooling. Nonetheless, years of neglect in the formalisation of the MATS curriculum and a lack of oversight in the quality of these schools have led to instances like the ones stated above.
Can MATS have a role in our healthcare system?
Doctors are often seen as the backbone of the healthcare system. However, the system relies on a range of professionals to function effectively. MATS graduates, as their name suggests, are trained to assist medical practitioners, and their skills fill critical gaps in Bangladesh's healthcare infrastructure, particularly in emergency and rural care. Globally, paramedics play a pivotal role in emergency response which significantly improves patient outcomes.
According to the World Health Organization (WHO), countries with robust paramedic systems have seen a reduction in preventable deaths caused by delays in emergency care. Bangladesh, however, lacks a standardised paramedic workforce. With proper training and regulatory frameworks, MATS graduates can become skilled paramedics, addressing both healthcare needs and unemployment among this group. For instance, India's introduction of paramedic training programmes under the National Skill Development Corporation (NSDC) has demonstrated how such initiatives can enhance healthcare delivery while creating employment opportunities.
Furthermore, integrating MATS graduates into the healthcare system aligns with the Sustainable Development Goals (SDGs), particularly Goal 3, which stresses universal health coverage and access to quality care. By leveraging their potential, Bangladesh can take a significant step towards building a more resilient and inclusive healthcare system. The protests, therefore, are a wake-up call for systemic reform that benefits both healthcare professionals and the population at large.
The dilemma of using "Dr"
On March 12, 2025, the High Court directed that only individuals who have completed their MBBS and BDS degrees can use the title "Dr". The court also clarified that those who previously used the title despite not completing MBBS or BDS degrees cannot be punished. However, any such use from the day that the verdict was ruled would be considered an offence under the relevant law.
The dilemma, however, over MATS graduates using the title "Dr" underscores a deeper struggle for recognition within the rigid professional hierarchy. While their demand reflects a desire for respect and validation, it also risks conflating their role with that of fully qualified doctors, potentially leading to confusion and ethical concerns.
The title "Dr" is not merely an honorific; it signifies years of rigorous medical training and expertise, which MATS graduates, despite their valuable contributions, have not undergone. Allowing them to adopt this title could inadvertently dilute its significance and undermine public trust in healthcare credentials. This issue is further complicated by the fact that even village doctors use the title "Dr" in some cases, despite receiving less standardised training than MATS graduates. Their use of the title has similarly sparked debates about professionalism and the integrity of medical credentials. This dual dilemma really accentuates a systemic issue: the lack of clear titles and career pathways for paramedical professionals in Bangladesh.

Instead of focusing solely on the title, the solution should lie in creating formalised roles and titles that reflect their expertise, such as "Paramedic Officer" or "Medical Assistant Specialist" for MATS graduates, and "Community Health Officer" for SACMOs. This approach would grant them the respect they deserve while maintaining the integrity of professional distinctions. Countries with advanced healthcare systems have successfully integrated paramedics into their frameworks, recognising their indispensable role in emergency and rural care without conflating their qualifications with those of doctors.
Ultimately, the fight for recognition should not be about a title but about creating a system that values their contributions and provides clear career pathways. Respect is earned not through prefixes but through the quality of service and the impact of one's work. What matters most is the value they bring to healthcare, not the letters before their name.
Mehrab Jamee is an activist at Sandhani and a fifth-year medical student at Mugda Medical College.
Purna is a third-year medical student at Shaheed M. Monsur Ali Medical College, Sirajganj. Send her e-mails at: ahnafpurna@gmail.com



 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel. 


Comments